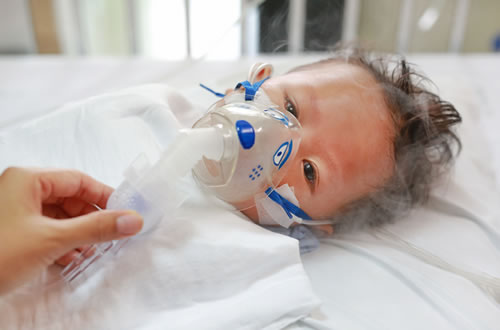
Respiratory Syncytial Virus or RSV is an illness found in children that can cause issues with breathing, it’s the most common cause of inflammation of the small airways in the lungs and pneumonia in babies.
What causes RSV?
It’s caused when a child touches a contaminated surface and then touches their eyes, mouth or nose, or by coming into contact with fluid from an infected person’s mouth or nose or inhaling droplets from a sneeze or cough from someone else.
It is often more common in the Winter or colder months and more likely when a child spends a lot of time around other children in childcare settings. Most babies are infected by the time they are 2 years old and can often be re-infected throughout their life.
What are the symptoms of RSV?
Symptoms usually start within 5 days after contact with someone with the virus. The early stages mirror that of common cold and can be quite mild, but with some children younger than 3, the illness can move to the lungs and often result in wheezing or coughing. In more severe situations, it can turn into a more serious respiratory disease and your child may need help with hospital treatment to help them breathe. It is of course advised that the child sees a healthcare provider to help diagnose the virus, but the most common symptoms to look out for are:
- Fever
- Cough
- Runny nose
- Trouble eating or drinking
- Wheezing in their chest
- Breathing faster than usual or having trouble breathing
- Fingertips and lips turn blue
- Apnea (short periods of not breathing)
How is RSV diagnosed in children?
RSV is usually diagnosed by a healthcare professional performing a physical examination on the child patient. For accurate diagnosis, a nasal swab may be taken to test the fluid from the nose for the virus.
Breathomics offers another, potentially more accurate way to diagnose respiratory infections. Imspex Medical’s Breathspec technology uses a combination of Gas Chromatography (GC) and Ion Mobility Spectrometry (IMS) which result in non-invasive breath analysis to more accurately screen and diagnose patients. Our studies of the technology have shown a sensitivity and specificity of 95% which means a faster diagnosis resulting in more accurate treatment.
In a recent article, Breath analysis for respiratory infections, authors including Cristina E. Davis say: “Over the last decade, there have been tremendous advances in breath analysis techniques applied to respiratory infection and colonization, which represents one of the most clinically relevant applications for the field of breath diagnostics and monitoring.”
How is RSV treated in a child?
Treatment will largely depend on the diagnosis and whilst there are ventilation solutions for those with a severe form of the virus or more obvious things like increasing fluid intake and suctioning of mucus, treatment with antivirals are often considered by healthcare professionals.
You may be familiar with the increasing attention being given to antimicrobial resistance whereby viruses, bacteria and fungi change over time and no longer respond to medicines we have been using for years. This makes infections harder to treat which increases the risk of diseases being able to spread.
We believe that through more accurate diagnosis of this type of respiratory virus or infection using breath biomarkers from breath analysis, that more accurate treatment can be prescribed preventing the spread and personalising healthcare for children that contract viruses like RSV.
RSV has symptoms that can often and easily be confused with other illnesses or respiratory tract infections when diagnosing through physical examination alone and generic antibiotics being prescribed will only aid the resistance.
To find out more about the technology used in Breathspec and some of our other solutions, click here.